As parents, many of us are mindful of how much sugar we give to our little ones, but what about their salt intake, especially if you’re following mixed feeding approach.
HOW MUCH SALT IS TOO MUCH?
Due to limited data for babies, an AI (Adequate Intake) for sodium has been established.
- For infants 6 months and younger, the AI for sodium is 110 milligrams per day (here).
- For babies between 7 and 12 months old, the AI increases to 370 milligrams per day (here).
This means that for babies under 12 months, the recommended sodium intake is less than 400 mg per day, which includes sodium from both breastmilk/formula and solid foods. Considering that breastmilk and formula contain around 200 mg of sodium per 24 oz., babies should only be consuming about 200 mg of sodium through solid food daily.
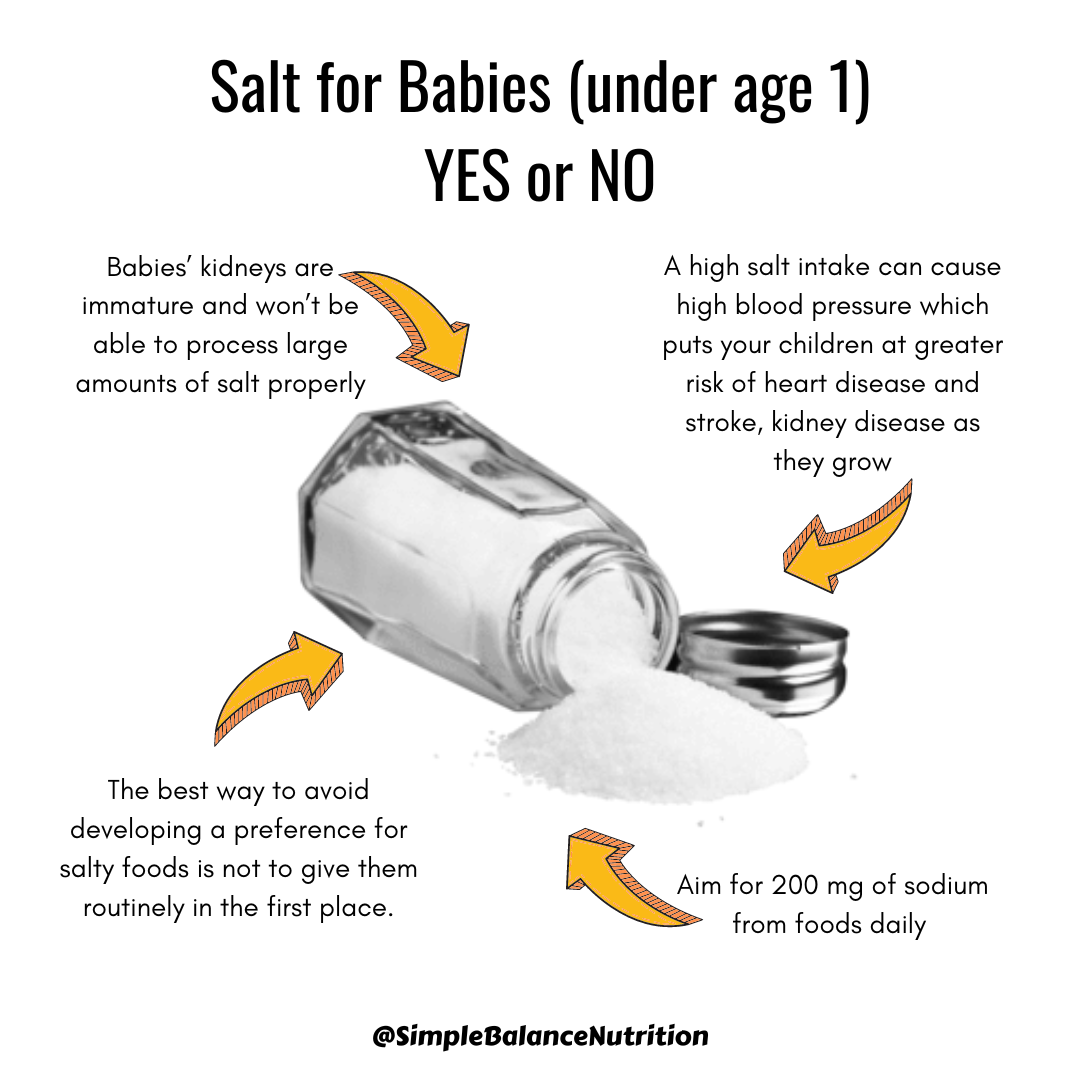
The reason for this recommended intake level is that we assume that babies’ kidneys are still very immature and may not be able to process large amounts of salt properly. While there isn’t enough research to definitively say that 400 mg is the maximum safe level for babies under 1 year old, it’s best to stick to this limit until more data is available. Exceeding this could potentially increase the risk of health issues, so erring on the side of caution is recommended.
SALT VS. SODIUM
Salt and sodium are often used interchangeably, and you may see both terms on food labels. However, table salt is actually composed of 40% sodium and 60% chloride.
1 teaspoon of salt = 2300 mg sodium
1 gram of sodium = 2.5 grams of salt
Both sodium and chloride are essential electrolytes (along with potassium) and play vital roles in the body. They help transmit nerve signals, enable muscles contractions, regulate fluids balance, enhance nutrient absorption, maintain acid-base balance, support potassium absorption, and control stomach bacteria levels.
SALT IN FOODS
Salt is found in almost all store-bought, processed, or packaged foods. It acts as a preservative and enhances flavor, so food manufactures often add it deliberately. Common foods that contain salt include:
- Processed meats like deli meats, bacon, hotdogs, ham, and sausages
- Frozen foods like fish sticks, chicken nuggets, and frozen meals.
- Potato chips
- Crackers
- Canned soups
- Gravy
- Broths (vegetables, chicken, beef)
- Olives, pickles, pickled vegetables (Kimchi)
- Soy sauce

Other foods that are high in sodium, even though they may not taste very salty, include:
- Cheese and other dairy products like yogurt and milk
- Bread, bagels, English muffins, tortillas, and other bread products
- Canned tomato and pasta sauce
- Canned vegetables
- Canned beans
- Boxed cereal
*Fresh Milk contains about 100 mg sodium per cup. This is one reason why milk is not recommended as the main drink for babies under one year old. However, a small amount of milk in cereal or baked goods is fine, so there’s no need to eliminate it completely.
WHAT SHOULD YOU DO?
As shown in the picture above, sodium is naturally present in many foods and is often added to processed foods. It’s found in nearly everything we eat. So do you need to completely eliminate salt from your baby’s solid foods?
AT HOME
When cooking meals for your family, you can hold off on adding salt until after you’ve taken out your baby’s portion. For example, when if you’re making a stir-fry, take out a small portion for your baby before adding soy sauce to the rest of the dish.
It’s important not to add salt to anything you prepare from scratch, even if you think it tastes bland. What may seem bland to you could be perfectly flavorful for your baby. Instead of salt,. try using herbs and spices as to enhance the flavor.
During the first few months of eating, it’s very unlikely that a baby will consume a large amount of sodium, especially if you’re mindful of the foods you provide. Since babies don’t eat that much in the beginning, it’s difficult for them to take in lot of sodium. Additionally, if your baby is self-feeding, it can take time for them to actually ingest a significant amount of food!
As you baby gets older and starts sharing more family-style meals, you’ll need to be more aware of their sodium intake, as hidden sodium can be found in many foods!
AT RESTAURANT
Restaurant foods tend to be much saltier than what you would make at home, and it’s hard to know exactly how much sodium is in a dish. Even if the nutritional information is available, chefs often add salt as they see fit, regardless of the recipe. Here’s how you can approach dining out with your baby.
Generally, I recommend not stressing too much about it. As long as you aren’t eating at a restaurant daily or multiple times a day, it will balance out. Try ordering dishes that are typically prepared with less salt, and don’t hesitate to ask the waiter’s or chef for suggestions.
If your baby isn’t eating much yet, or if they tend to eat small portions, you should be fine. However, if your baby has a good appetite, consider bringing some low-sodium food for home. Personally, I find that I can usually make do with what’s on the menu, and I want my child to experience a variety of flavors. But if you’re unsure, bringing your own is always a good backup.
The key is to be mindful and balance things over the next few days. For example, if one day your baby eat a a lot of cheese and bread, you can focus on offering low or no sodium foods the next day. If they eat a meal at a restaurant, you might serve fruit and a homemade muffin for their next snack.
Pick your battles and make the best choices you can. If you only eat out once or twice a week, just adjust your baby’s food choices for the rest of the week! Keep it truly balanced while continually striving to plan ahead.
BOTTOM LINE
Do your best to serve homemade meals whenever possible. Read labels and be mindful of what you and your baby are eating. This is a healthy habit for the entire family.