My specialty? Working alongside parents to revolutionize how they feed their children and how their children eat. Together, we can empower your children to embrace new foods, enjoy a diverse range of options from various food groups, sit down to meals happily without any battles, and cultivate a lifelong healthy relationship with food and their bodies.
If you’re ready to dive in and work with a pediatric dietitian one-on-one, you can book an appointment with me right here. Whether you’re dealing with picky eating, a child seemingly “addicted to sugar,” weight concerns, or just need help getting nutritious meals on the table, you’ve come to the right place.
In this post, I’ll walk you through what a pediatric dietitian does, why it’s crucial to seek out a specialist in pediatric nutrition for your children, and how you can go about finding one. Plus, I’ll give you a sneak peek into what you can expect when working with a pediatric dietitian, so you can be confident in finding the perfect fit for your family.
So, if you’re ready to kickstart your journey towards happier, healthier eating habits for your children, let’s get started!
WHY CHILDHOOD NUTRITION IS IMPORTANT

The global obesity crisis has worsened in recent years, with research pointing out how more and more children deal with this harmful condition. Pediatric dietitians and nutritionists are here to help prevent children from developing unhealthy body mass indexes and to support those who are on their weight loss journey.
A century ago, the notion of a child needing a dietitian would have been met with skepticism. Back then, the food they ate was generally more nutritious and less processed. Plus, the idea of seeking professional guidance for children’s diets wasn’t widely accepted.
Fast forward to today, we are dealing with more obese children than ever with pre-diabetes and diabetes, inflammatory bowel syndrome, autoimmune diseases, skin issues, and a variety of food intolerances and allergies. It’s a serious global issue that demands attention.
Despite the gravity of the situation, the importance of addressing children’s dietary preferences and involving pediatric dietitians in the conversation has become increasingly evident. Parents are recognizing the significance of seeking expert guidance to ensure their children’s nutritional needs are met and to tackle health challenges head-on.
In essence, while the prevalence of childhood obesity presents a significant challenge, the role of pediatric dietitians has never been more crucial. By working together to promote healthier eating habits and address nutritional concerns, we can strive towards a healthier future for our children.
WHAT DOES A PEDIATRIC DIETITIAN DO?

A pediatric dietitian is dedicated to collaborating with children and their families to enhance their dietary habits, nutrition, and feeding routines. There are various reasons why a child might benefit from consulting a pediatric dietitian, which I’ll delve into below.
During the initial consultation with a pediatric dietitian, a comprehensive nutrition assessment is conducted. This typically involves:
- Reviewing the child’s medical history in detail.
- Assessing growth parameters such as height, weight, and growth charts to track progress over time.
- Evaluating the child’s weight and height history to identify any trends or concerns.
- Gaining insight into the child’s typical dietary intake and preferences.
- Engaging in thorough discussions and asking pertinent questions to better understand the child’s unique needs and circumstances.
Based on this assessment, the pediatric dietitian will develop dietary modification recommendations and work closely with the family to implement these recommendations effectively. The frequency and duration of follow-up visits will vary depending on the individual needs of the child.
Overall, the primary goal of a pediatric dietitian is to support children and their families in optimizing their nutritional intake, fostering healthy eating habits, and addressing any dietary concerns or challenges they may encounter along the way.
WHEN TO SEE A PEDIATRIC DIETITIAN
Wondering when it’s time to seek guidance from a pediatric dietitian? Here are some common scenarios where their expertise can make a significant difference:
1. Picky Eating

If mealtimes at your home resemble battlegrounds due to a picky eater, a dietitian can offer valuable support. They can help alleviate mealtime stress and create strategies to encourage your child to explore new foods. Picky eating is often seen in toddlers and preschoolers but can persist if left unaddressed, potentially impacting growth. Early intervention with a dietitian’s comprehensive assessment can help set your child on the right path. Check out my online course PEACEFUL MEALTIMES to help your children start trying new foods.
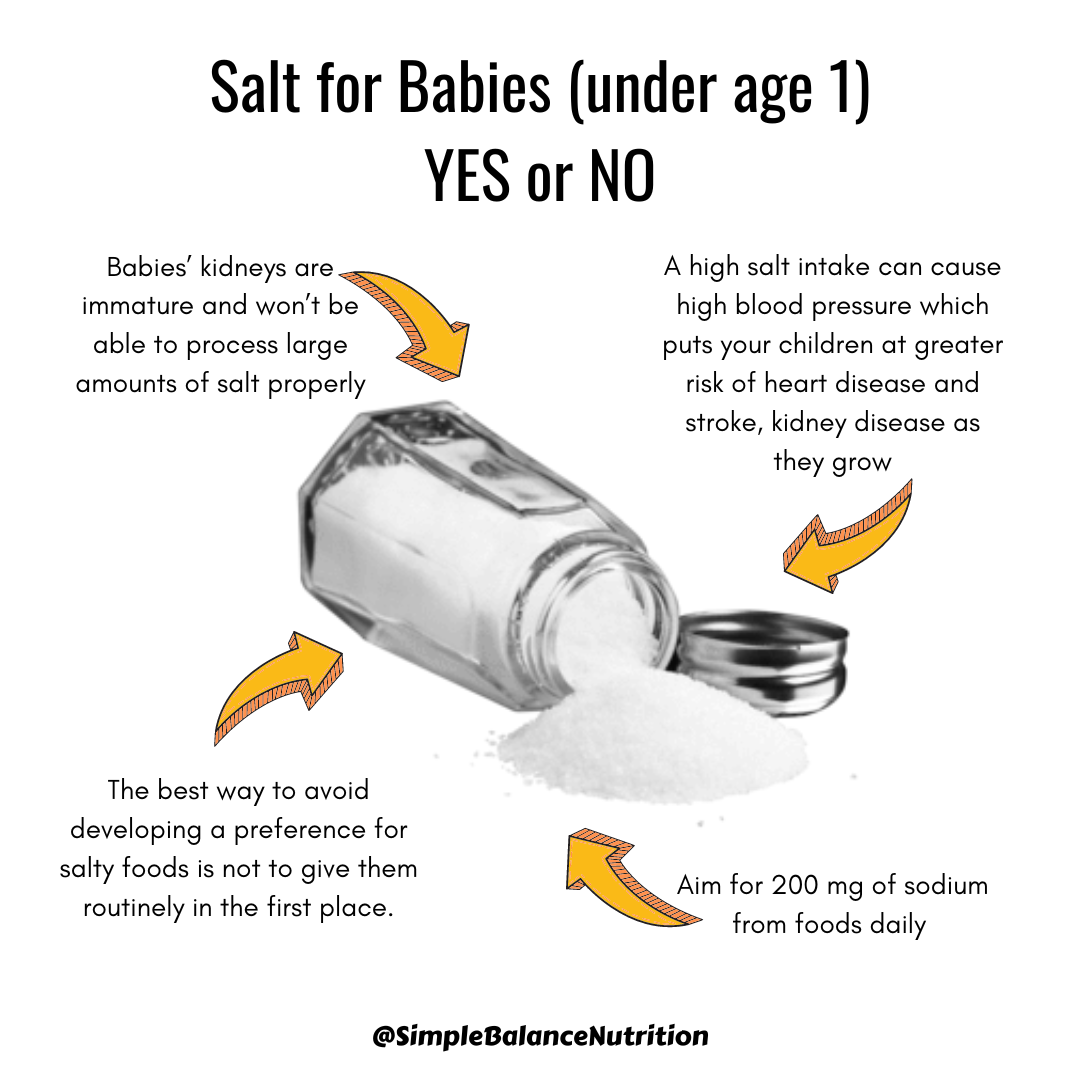
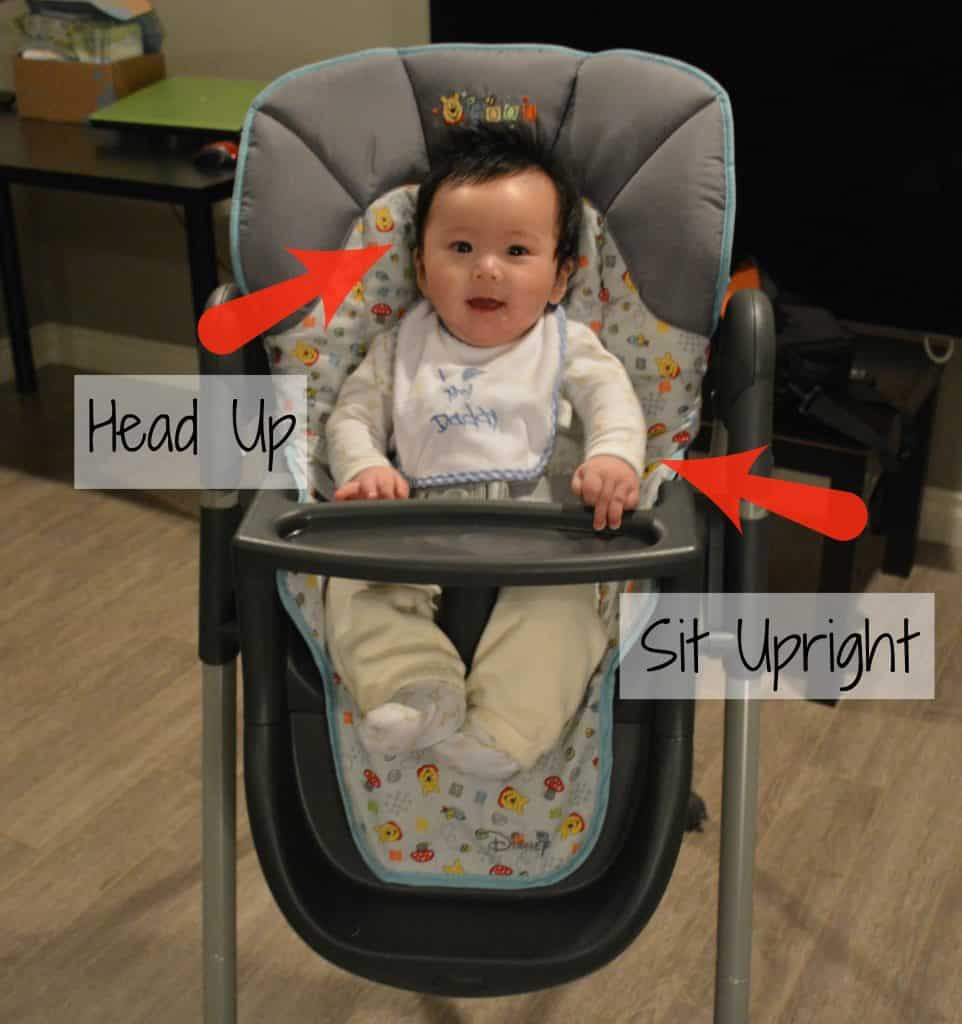
2. Starting Solids and Baby-Led Weaning

Navigating the transition to solid foods can be daunting for new parents. A dietitian can provide guidance on your baby’s nutritional needs, appropriate food choices, and transitioning through different textures. For those considering baby-led weaning, a dietitian can offer tailored advice and meal ideas to support this approach.
3. Nutrient Deficiencies

If your child is diagnosed with a nutrient deficiency, such as iron or vitamin D, a dietitian can help rectify the imbalance through dietary adjustments or supplements. Iron deficiency, particularly common in toddlers consuming excessive milk alternatives, requires careful management to restore optimal levels.
4. Constipation

Constipation is a prevalent issue in children, often influenced by diet. A dietitian can analyze your child’s dietary habits and recommend adjustments to promote regular bowel movements. They may suggest incorporating probiotic-rich foods or supplements and offer easy-to-follow recipes for constipation relief.
5. Child Athletes

Proper nutrition is vital for young athletes to support performance, recovery, and growth. A dietitian specializing in pediatric nutrition and sports can provide tailored guidance to optimize your child’s nutritional intake, considering their high activity levels and rapid growth.
6. Weight Concerns

If there are concerns about your child’s weight or growth, a pediatric dietitian can conduct a comprehensive assessment to determine if intervention is necessary. It’s essential to approach discussions about weight sensitively and privately, focusing on overall health rather than appearance to prevent negative associations.
7. Food Allergies

Children with food allergies may require guidance to ensure they receive adequate nutrients while avoiding allergens. A dietitian can assist in identifying suitable alternatives and designing a balanced diet that meets their nutritional needs.
8. Other Health Concerns

There are numerous other reasons to consult a pediatric dietitian, including general growth and nutrition concerns. If you have any concerns about your child’s diet or nutrition, consider discussing them with their pediatrician to explore the possibility of a referral to a dietitian.
Remember, the expertise of a pediatric dietitian can play a pivotal role in addressing various dietary challenges and promoting optimal health and well-being for your child.
When seeking a pediatric dietitian to address your child’s nutritional needs, consider the following avenues:
By exploring these avenues and seeking referrals from trusted sources, you can connect with a qualified pediatric dietitian who can address your child’s unique nutritional needs and support their health and well-being.
A pediatric dietitian is a registered dietitian specializing in working with children, equipped with extensive experience in pediatric nutrition. They offer invaluable support and guidance across various nutrition-related challenges, including picky eating, introducing solids, weight and growth concerns, addressing nutrient deficiencies, and devising healthy meal plans tailored to children’s needs.
Whether you opt for a local or virtual dietitian depends on your specific circumstances and preferences. The crucial factor is finding a professional with a solid background in pediatric nutrition, ensuring the best possible care for your family.
With over 13 years of dedicated experience in pediatric nutrition, I’m here to support you every step of the way. Whether you’re ready to schedule a consultation or simply have questions about your child’s nutrition, feel free to reach out. I offer a range of free resources to kickstart your journey towards better health and nutrition for your child.