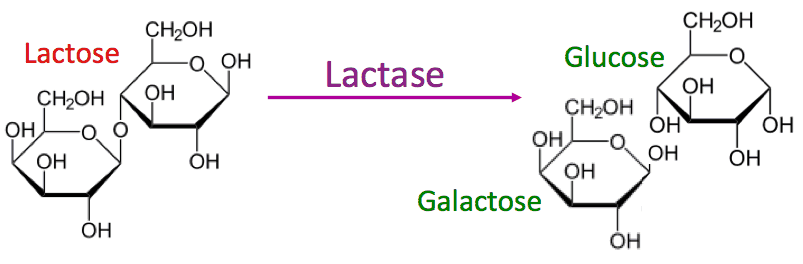
The immune system plays a very important role in protecting both adults and children from infections. It’s made up of a highly interconnected network of white blood cells, antibodies, bone marrow, the spleen, thymus and the lymphatic system. Together, these systems identify and destroy harmful invaders like viruses and bacteria.
With Covid-19 and seasonal illness in the spotlight, many parents have searched for ways to “boost” their child’s immunity. But here’s the truth:
There’s no magic supplement, product, or food that can “boost” the immune system.
In fact, an “overactive” immune system is linked to autoimmune diseases like lupus or multiple sclerosis. The term immune boosting is a marketing phrase, not a medical one. Instead, what matters most is supporting the immune system so it functions normally and effectively.
THERE IS NO SINGLE PRODUCT THAT CAN BOOST IMMUNITY
Scientists are still uncovering how all the pieces of the immune system work together. While we can’t “boost” it, we can provide the right conditions for it to thrive.
There are many things we can do to “support” immunity, such as getting enough sleep, being physically active, minimizing stress and eating nutritious foods. As a busy mom, I love finding foods that are not only nutritious and convenient, but also immune supporting.
The easiest way to get these nutrients is by eating a healthy and balanced diet.
Certain nutrients, such as zinc, selenium, iron, protein, vitamins A, C, D and E are critical for the function of immune cells. However, I can’t promise you that you can totally shield your children from getting sick by eating foods with these nutrients. In fact, you can build up your children’s immune systems with nutrient-dense foods. Certain foods have the exact nutrients that can help your children’s immune systems be as strong as possible, so when they are exposed to the inevitable germs, they are ready to fight.
NUTRIENTS & FOODS THAT SUPPORT IMMUNITY
Let’s dive into some of the foods and nutrients that play an important role in immune health.
Orange Vegetables and Fruits
Carrots, sweet potatoes, pumpkin and cantaloupe are rich in beta-carotene, a precursor of vitamin A. Beta-carotene has several health benefits, including the antioxidant activity that protects cells from free radical damage and help enhance immune function (here). In fact, beta-carotene helps form white blood cells, which track down and destroy pathogens.
Pairing these foods with a healthy fat, such as olive oil, avocado, or nuts and seeds, can help your child absorb the nutrients more effectively.
Berries
Berries are packed with antioxidants that reduce oxidative stress and keep immune cells functioning well. Strawberries, blueberries, raspberries, cranberries, and blackberries – fresh or frozen. Add them to yogurt, oatmeal, or enjoy as snack.
Dark leafy greens
Kale, spinach, bok choy and gailan contain carotenoids, another antioxidant group linked with immune health. If your children not a fan of salads, just blend them into smoothies, stir into pasta sauces, or add to muffins.
Nuts
Almonds, peanuts and hazelnuts contain vitamin E, which helps increase T-cell count (T-cells directly kill infected host cells and regulate immune responses) (here).
Walnuts also stand out for their omega-3 fats. Offer a mix for variety, but remember: for toddlers, use thin nut butter spreads or finely chopped/slivered nuts to reduce choking risk.
Seeds
Pumpkin, sunflower, sesame, hemp, and flax seeds contain vitamin E, zinc, and omega 3 fatty acids.
Sprinkle on yogurt, blend into smoothies, or spread seed butter thinly on toast.
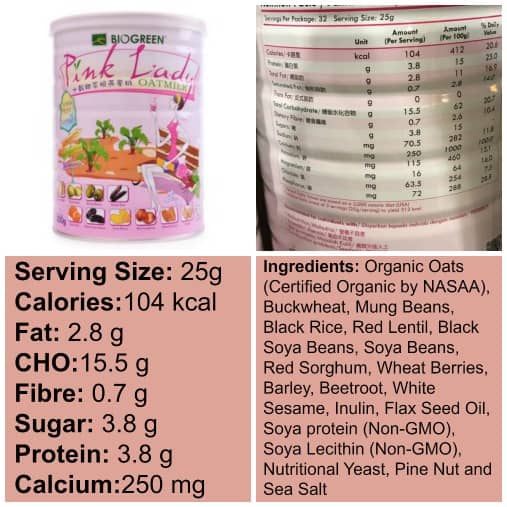
Oatmeal
Oats contain immune-supporting nutrients like selenium and zinc. But they also contain a special type of fibre called beta-glucan, which increases immune defense by enhancing macrophages (cells that detect and destroy bacteria and viruses) (here). A warm bowl of oats makes an easy immune-supporting breakfast.
Eggs
Eggs are a high-quality protein source, often used as the gold standard for measuring protein quality. Eggs contain selenium and vitamins A, D and E, all important for immune cell development and function.
Fatty Fish
Salmon, tuna, trout or sardines provide vitamin D and omega-3 fats. Vitamin D deficiency is linked to higher infection risk (here), while omega-3 fats are part of the structure of all immune cells (here). Try canned tuna in a sandwich or salmon in sushi rolls.
Fermented Foods
Kefir, fermented vegetables (sauerkraut or kimchi), kombucha and yogurt contain probiotics that support gut health, which is closely tied to immune function (here). While research continue to identify which probiotic strains are most helpful, including fermented foods is a safe and beneficial choice.
Tumeric
This golden spice contains curcumin, which has been linked to enhance immune responses. Because curcumin isn’t easily absorbed, pair it with black pepper to increase bioavailability by up to 2000% (here). Use in curries, soups or even a turmeric latte, known as golden milk.
HYDRATION MATTERS TOO
Water helps regulate body temperature, keeps cells functioning properly, and supports the clearance of irritants from the lungs and nasal passages. Especially in hot, humid climates like Malaysia, staying hydrated is essential for immune health.
SEASONAL FLU SHOT
One important way to help protect children from getting seriously sick is the seasonal flu shot. Because flu viruses change from year to year, the vaccine is updated annually to match the strains most likely to circulate. That’s why experts recommend getting the flu shot once every year, usually before the flu season starts. While it doesn’t “boost” the immune system in the way marketing often suggests, it does train the immune system to recognize and fight the flu more effectively, reducing the risk of severe illness, complications, and hospitalisation in children.
WHAT ABOUT PROBIOTIC SUPPLEMENTS
Currently, there isn’t enough strong evidence to recommend routine probiotic supplements for children. Not all probiotic strains have the same effects, and in some cases, the wrong strain could suppress immunity instead of supporting it. For most families, probiotics from food sources are the safest and most beneficial option.
BOTTOM LINE
You don’t need a special pill, powder, or “immune-boosting” food to protect your child. Instead, focus on the basics:
- A balanced, varied diet rich in fruits, vegetables, protein, and healthy fats
- Enough sleep, physical activity, and hydration
- Including a mix of the nutrient-dense foods above in daily meals
These habits won’t prevent every cold or flu, exposure to germs is part of childhood. But they will give your child’s immune system the support it needs to respond effectively.
If mealtimes with your little one often feel like a battle, you’re not alone. My online class Peaceful Mealtimes is designed to give you practical tools, proven strategies, and confidence to help your child eat better without the stress and power struggles. Join today and bring calm back to your family table.
Update: August 25, 2025